3billion Reanalysis Part 2 : New Clinical Information Can Change the Diagnostic Direction
In clinical practice, we are reminded of one simple truth again and again:
Genomic test results are not static. As a patient’s clinical information evolves, the meaning of their genomic data can change as well.
This is exactly where the importance of phenotype updates begins.
Across many studies, one finding consistently stands out — when new clinical information is added, the diagnostic yield of reanalysis increases.
Sometimes, just a few updated lines from a clinician become the critical clue that leads to a diagnosis that had remained elusive for years.
In this article, we explore how phenotype updates function as a powerful tool in reanalysis at 3billion, and how we have incorporated and optimized this approach in our workflows.
Why Do Phenotype Updates Increase Diagnostic Yield?
Across many studies, one conclusion consistently emerges:
When new clinical information (phenotypes) is added, the efficiency and success rate of reanalysis increase.
This improvement is not simply due to advances in analytic technology. It happens because the medical context becomes richer.
For example, consider a patient who initially presented only with “developmental delay,” but later develops seizures, visual abnormalities, or ataxia during follow-up.
In such cases:
→ The same genetic variant can be interpreted in a completely different way, and
→ Variants that previously seemed uncertain may now emerge as strong candidates for pathogenicity.
Reference
Fung JLF, et al. (2020). A three-year follow-up study evaluating clinical utility of exome sequencing and diagnostic potential of reanalysis. NPJ Genom Med. 2020 Sep 10;5(1):37.
Ji J, et al. (2021). Clinical Exome Reanalysis: Current Practice and Beyond. Mol Diagn Ther. 2021 Sep;25(5):529-536.
The Two Most Effective Ways to Share New Clinical Information
Phenotype updates are one of the most powerful clues in reanalysis. At 3billion, there are two effective ways to provide this information:
1️⃣ Share the update with your sales representative
This is the simplest option. Once the information is received, it is quickly relayed internally to our clinical genetics team.
2️⃣ Update the information directly through the 3billion Portal
This is the most accurate and structured method. Portal updates ensure that the clinical team has the most precise information when making diagnostic decisions during reanalysis.
Advantages of updating through the Portal:
- All changes are immediately reflected in the system, minimizing the risk of missing information
- You can add the most appropriate and specific HPO terms
- You can directly specify requested genes
- File uploads are supported
- Additional clinical notes can be included for detailed communication
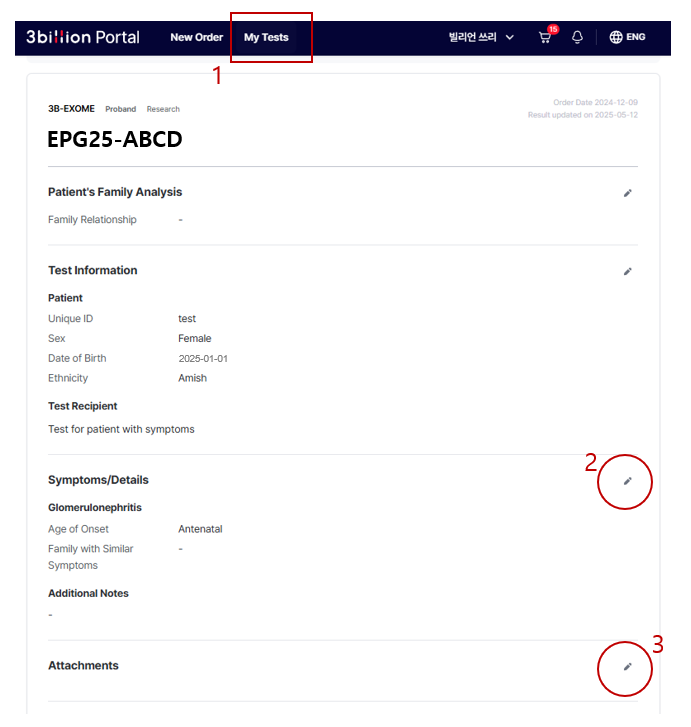
- Go to the My Tests menu and select the sample you want to update.
- Click the edit icon in the Symptoms/Details section to add or modify clinical information needed for reanalysis.
- Use the edit icon in the Attachments section to upload any files you would like to share for reanalysis.
What Happens Inside 3billion After You Update the Information?
Once new clinical information is added, it is immediately integrated into the patient’s data. From there, our internal analysis pipeline automatically initiates reanalysis.
The core of this process is 3ASC.
3ASC reprioritizes variants based on the newly added phenotypes as well as the most up-to-date literature and databases.
In other words, it automatically selects the variants that best explain the updated clinical presentation.
After this automated step, our clinical genetics team reviews the full data set and updates the final interpretation.
How We Notify You of Reanalysis Results
- If a clinically significant variant is identified:
You will receive an updated reanalysis report. - If no significant findings are identified:
You will receive an email informing you that reanalysis has been completed.
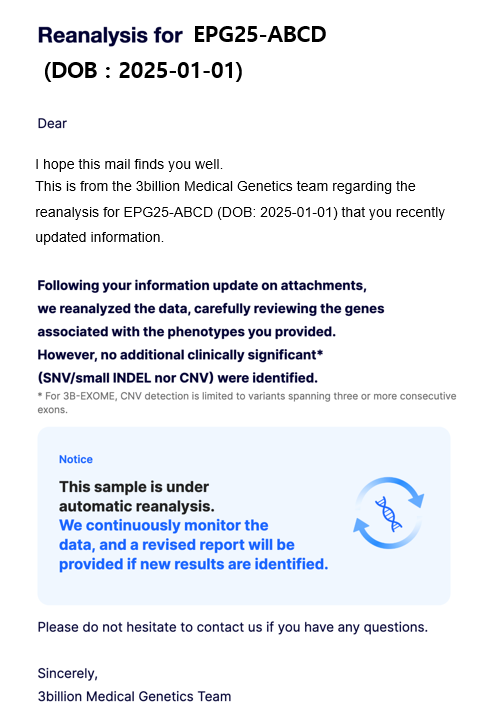
When Requesting Reanalysis, Which Updates Are Truly Helpful?
After ordering a genomic test, clinicians often notice new findings over time and request reanalysis. However, not all clinical updates are meaningful for reanalysis.
So here, we summarize which types of information genuinely help — and which ones do not.
❌ Updates That Generally Do Not Help Reanalysis
If the new information simply rephrases an existing symptom or adds minor descriptive detail, it is very unlikely to change the reanalysis outcome.
❌ Example 1
- Previous: Hearing impairment
- Update: Hearing loss, sensorineural
→ The patient already had hearing issues; the terminology is just more specific.
→ The overall disease category does not change, so the need for reanalysis remains low.
❌ Example 2
- Previous: Generalized hypotonia
- Update: Muscle weakness, generalized
→ Hypotonia and generalized muscle weakness overlap significantly in clinical context.
→ The differential diagnosis does not meaningfully change.
Updates that only “change the wording” provide little to no additional diagnostic value.
If the update does not reflect a new system involvement or a fundamentally different symptom, reanalysis will rarely alter the result — and may even reduce efficiency.
✔️ Updates That Are Truly Valuable for Reanalysis
The following types of updates can change the genotype–phenotype matching itself, increasing the chance that reanalysis will yield new findings.
✔️ Example 1 — Newly emerged neurological symptoms
- Previous: Global developmental delay, Hypotonia
- Update: Epileptic seizures (first onset at 2 years)
→ The onset of seizures is a new neurological clue and may strongly point toward a different gene set.
✔️ Example 2 — New evidence of organ involvement
- Previous: Failure to thrive, Mild hypotonia
- Update: Cardiomyopathy (echo: LV dilation)
→ Newly detected cardiac involvement represents a new organ system, shifting the diagnostic category entirely.
✔️ Example 3 — New test results suggesting a different diagnosis
- Previous: Hypotonia, Feeding difficulty
- Update: MRI: delayed myelination → suspicion of leukodystrophy
→ The phenotype category changes, which can alter the interpretation of previously identified variants.
In short: Reanalysis is most effective when a truly new clue appears.
In these situations, the chances of changing the diagnosis or reclassifying a VUS are significantly higher.
Reanalysis Is Possible Even Without Symptom Changes—But the Key Is When You Do It
So far, we’ve discussed why phenotype updates matter. Naturally, when a new phenotype appears, a reanalysis request is essential.
But in clinical practice, we often hear this question:
“Can we request reanalysis even if the patient’s symptoms haven’t changed?”
The short answer is: yes, you can.
Even when clinical features remain stable, the scientific landscape does not.
Literature and databases are continuously updated. New gene–disease associations are discovered, and variants once considered uncertain may be reclassified over time.
However, there is one important consideration: the timing of reanalysis.
Based on multiple studies and clinical experience, reanalyzing approximately every 2–3 years is known to be the most effective interval.
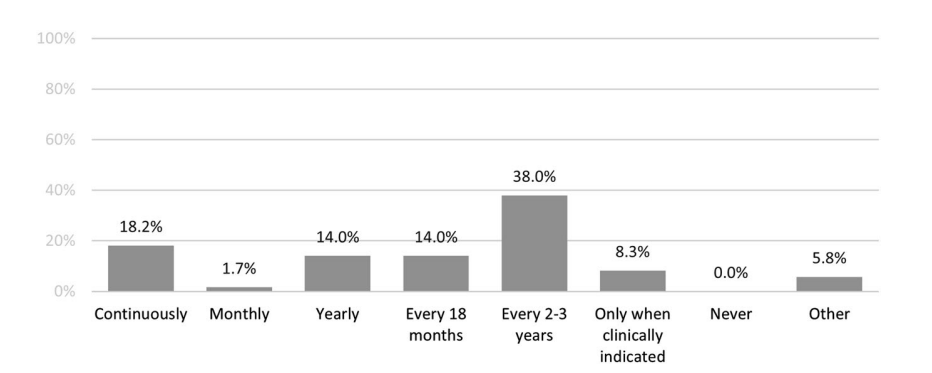
If reanalysis is repeated too frequently — for example, within just a few months — there is usually not enough change in the literature or databases to meaningfully affect the results.
In other words, what matters is not how often you reanalyze, but whether you do it at the right time.
Reference
Tan NB, et al. (2020) Evaluating systematic reanalysis of clinical genomic data in rare disease from single center experience and literature review. Mol Genet Genomic Med. 2020 Nov;8(11):e1508.
Best S, et al. (2024) Reanalysis of genomic data in rare disease: current practice and attitudes among Australian clinical and laboratory genetics services. Eur J Hum Genet. 2024 Nov;32(11):1428-1435.
In the End, the Heart of Reanalysis Is Collaboration
Reanalysis is not driven solely by technology or accumulated knowledge.
The clinician — who understands the patient’s evolving condition better than anyone — plays a critical role. Clinicians provide updated phenotypes and clinical information, and the genomic analysis team uses these updates to perform an accurate and informed reanalysis.
When this collaboration works seamlessly, the diagnostic yield of reanalysis reaches its full potential, allowing us to deliver the most precise and meaningful results to patients.
In the next article, we will introduce real cases where phenotype-based reanalysis directly led to a diagnosis.
Curious about reanalysis?
Explore more insights from 3billion’s clinical geneticists.
- 3billion Reanalysis Part 1: Genetic Testing Is Not the End — Why Is Reanalysis Necessary?
- 3billion Reanalysis Part 2 : New Clinical Information Can Change the Diagnostic Direction (Current Post)
- 3billion Re-analysis Part 3: Clinical Updates Expand Diagnosis – Case Sharing
- 3billion Re-analysis Part 4: The Geneticist’s “Third Eye”: AI Automated Reanalysis for New Diagnostic Insights
- 3billion Re-analysis Part 5: Bringing a Nearly Missed Diagnosis Back Into Focus – How 3ASC Redefined Automated Reanalysis
Get exclusive rare disease updates
from 3billion.

Sohyun Lee
Clinical Genomics Scientist & Clinical Customer Support — guiding test selection, supporting variant and result interpretation, handling case inquiries, and translating field insights into service improvements.






